Serum PSA Test for Prostate Cancer Screening - Do it Only if You Have the Physical Resources and Mental Make-Up to Handle the Consequences
Do a serum PSA test only if you can handle the consequences of an abnormal result

A 68-years old doctor friend of mine went for a whole body check-up. A serum prostate-specific antigen (PSA) test was done as part of the check-up. It was found to be abnormal. The value was 7 ng/ml. He went to a urologist who asked for a prostate MRI, which showed a suspicious lesion, which was then biopsied under ultrasound guidance using a trans-rectal approach. It turned out to be a Gleason 4+3 (7) cancer. He then had a PSMA-PET/CT that did not show spread outside the prostate. He was then offered a choice of surgery, radiotherapy or active surveillance. Within the surgery and radiotherapy groups, there were even more choices. Despite being a doctor and knowing good prostate cancer specialist doctors, some of whom were friends, he was thoroughly confused. Active surveillance? Which means monitoring serum PSA levels and doing regular prostate MRIs and then deciding on treatment, if there is progression? Surgery? Which type of surgery? Robotic? What about the complications? Radiotherapy? Which type? Isn’t radiotherapy a shade not as good as surgery? It’s been three months and he still hasn’t decided, which means at least currently he has subconsciously chosen active surveillance.
Decision making is not easy. The age of the patient, the grade of the tumor, the serum PSA level, the doctors you see, the resources available…all matter.
But the one question he keeps asking is…what if I had not done the serum PSA level in the first place?
At autopsy, a third of people above the age of 70 have asymptomatic prostate cancers [1], the incidence increasing to more than half in those over the age of 80 [2]. Which means that as men age, a few foci of cancer in the prostate are part of the ageing process and rarely if ever manifest clinically or cause symptoms or need treatment.
If you don’t do a serum PSA level, then like with most cancers in the body, you will come to know of your prostate cancer, if you develop one, only if and when you have symptoms. For some, it may turn out to be a late-stage diagnosis with reduced survival, but for the vast majority, it will not change longevity, the older you are at the time of diagnosis.
So it makes logical sense to then do a serum PSA level at regular intervals, and knock off the cancer early, if the PSA is found to be abnormal. Unfortunately, that logic does not work in real life.
Let’s say your PSA level is 6 ng/ml during a health check-up and you are asymptomatic. You first have to do nothing except wait for a couple of weeks to a month to repeat the test to check whether the raised level is real or not…till then you have to live with that thought in your mind that you may have prostate cancer…which again is not something that you may be able to handle.
If your repeat serum PSA level remains 6 ng/ml, you will then need to do a prostate MRI. If the MRI shows a possible or definite cancer, you will then need to undergo a biopsy, which is not without its own set of complications. Even if a prostate cancer is picked up, you will not really know, unless you decide to do nothing or choose active surveillance, whether this cancer is one of those that would have killed you.
Statistically, while serum PSA testing globally has reduced the rate of prostate cancer deaths wherever implemented [3], this has come at the cost of over-diagnosis and over-treatment of patients, who perhaps would not have needed treatment in the first place. Even with active surveillance, there is a mental cost to living with a so-called cancer that needs to be looked at every now and then. If you decide to get the cancer out, both surgery and radiotherapy are not without their complications.
It’s a tough choice and there are no easy answers.
One of the challenges of any screening program is how to maximize the health benefits of the screening program without causing harm or iatrogenic disease.
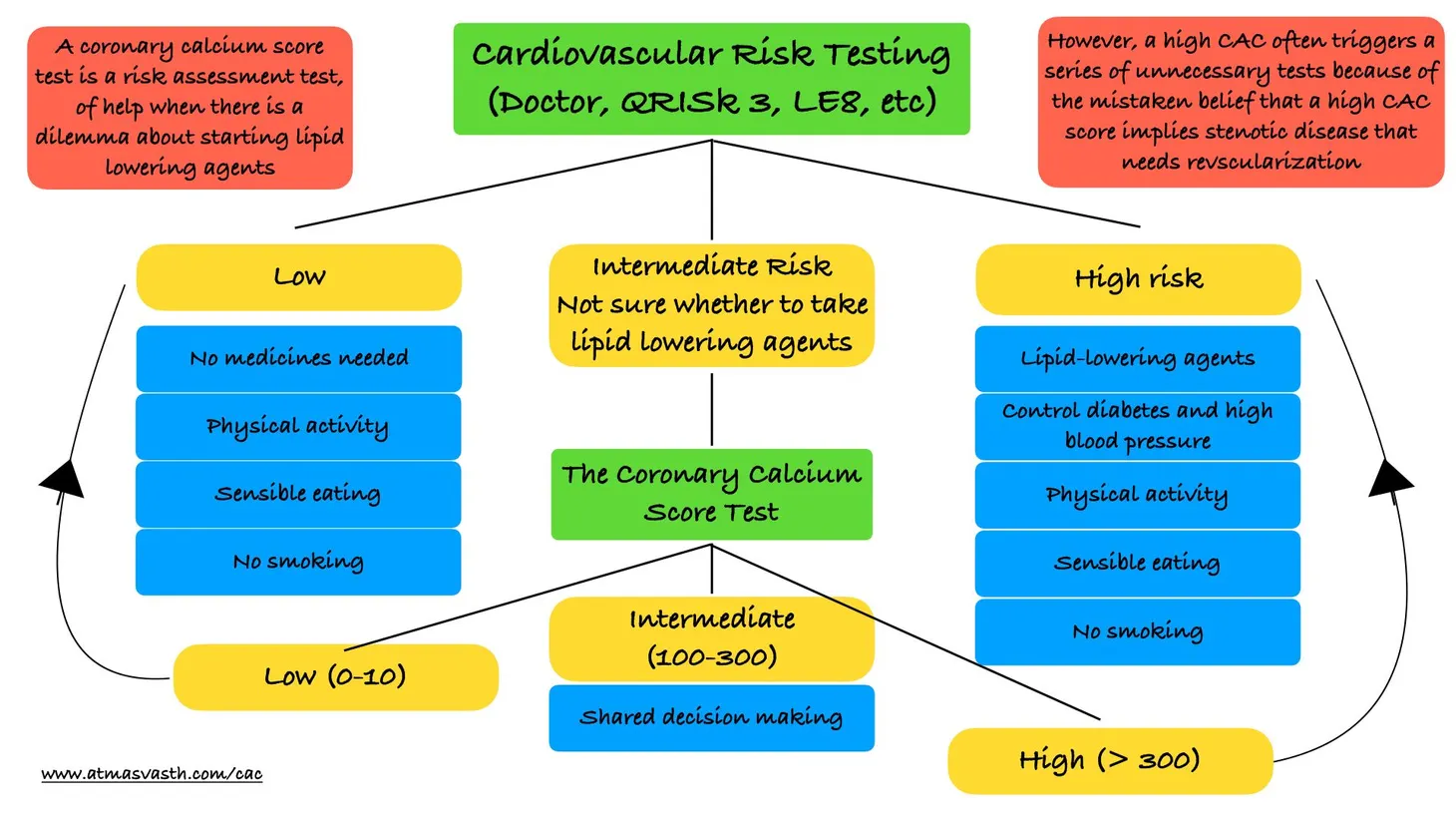
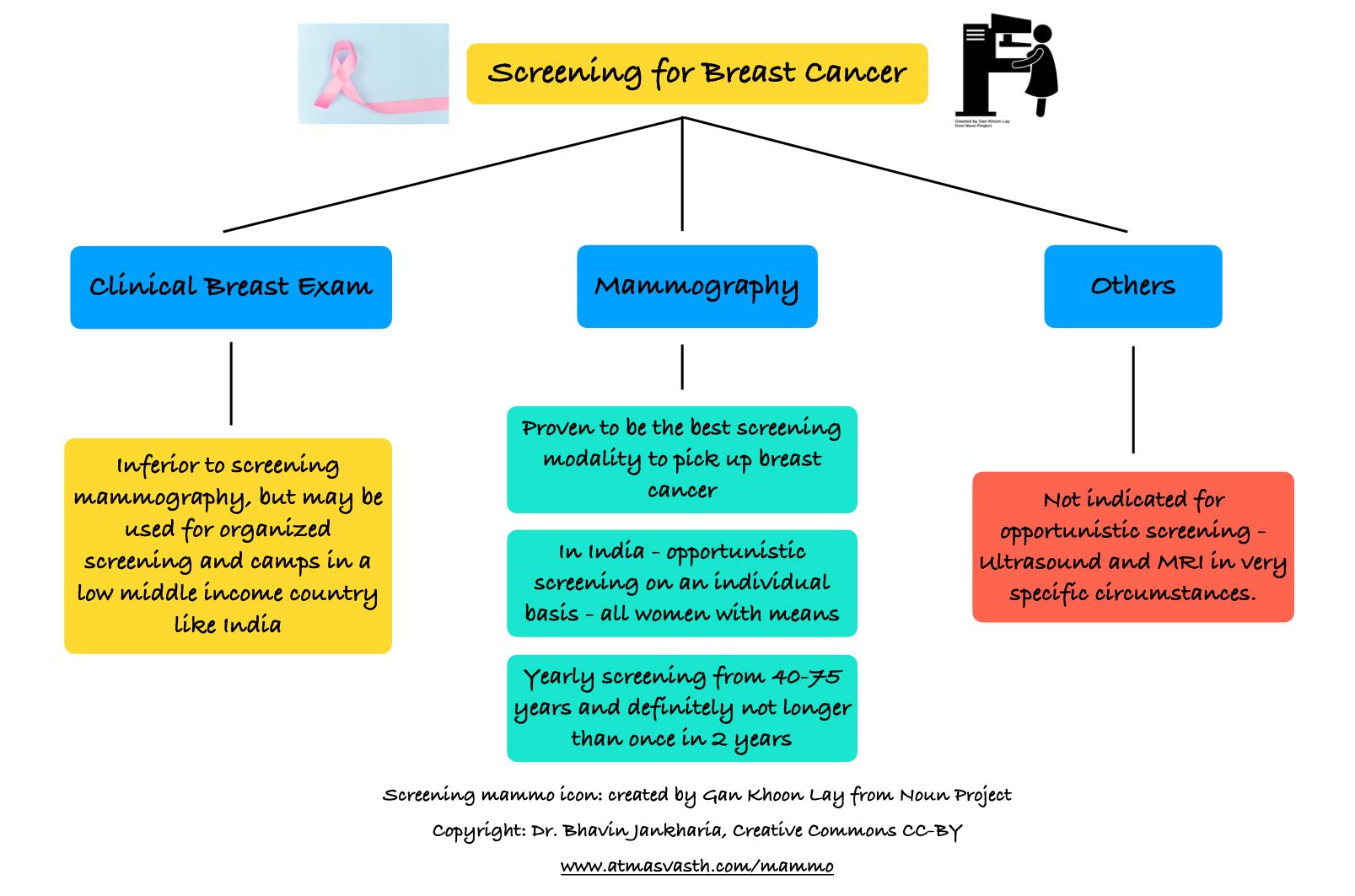
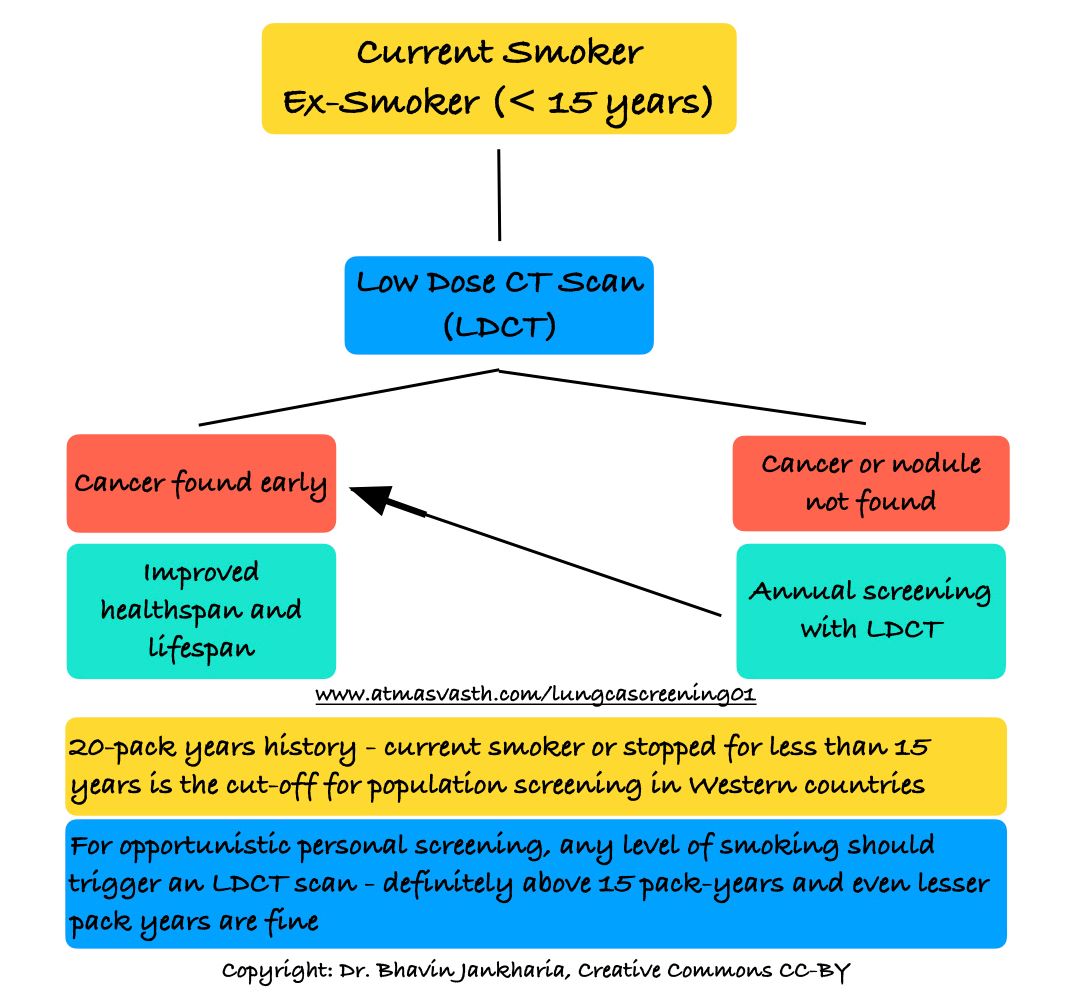
Screening mammography for breast cancer in women does precisely this - it saves lives without causing undue harm. Screening low dose CT for lung cancer in smokers also does more good than harm. Screening for cancer of the cervix make a huge difference. Non-oncology screening for diabetes, high blood pressure and cardiovascular risk, identifies disease early and allows prompt treatment, saving lives.
Prostate cancer screening is not in the same bucket, which is why the United States Preventive Services Task Force (USPSTF) guidelines [3] recommend against screening for those over 70 years of age and screening only as a shared decision between you and your doctor if you are between 55 and 69 years of age, after understanding all the pros and cons and the consequences of a raised PSA level.
In India, there is no public screening anyway, so the question of Govt or institution mandated screening does not arise. However, serum PSA testing is “thrown in” during executive health check-ups, as part of a panel of tests or is often advocated by hospitals and diagnostic centres to “rule out”cancer, because of the simplistic understanding that “early cancer detection saves lives”. Early detection does save lives, but only with a select group of cancers such as oral cancer, breast cancer, lung cancer in smokers, cancer of the cervix and those genetically predisposed to cancers.
Prostate cancer is just the 12th commonest cancer in India [4] accounting for 14% of all cancer deaths. The low incidence and prevalence are likely because screening with serum PSA is still performed only in middle to high income groups. Prostate cancer is predominantly a cancer of older men…only 1.5% of India’s population consists of men above the age of 70 years.
An Expert Group Consensus Opinion out of India headed by Amit Ghose [5] in 2019, though funnily published in the Korean Journal of Uro-Oncology, also recommends against prostate cancer screening in India for pretty much the same reasons.

So what should you and I do?
1. If you are above 70 years of age, please don’t do a serum PSA level. It is pointless. The older you are the more pointless it gets.
The 79-years old father-in-law of a friend of mine was found to have a mildly high serum PSA level 3-4 years ago, during an executive health check-up. He had a prostate MRI, which was normal. A year later, the serum PSA level had increased a bit. He had another prostate MRI, which was also normal. The same thing happened in the third year. The children could not believe that modern medicine could not find a cancer when the serum PSA was climbing and then decided to do a PSMA-PET/CT, at which time, the asymptomatic person (you can’t call him a patient when he does not have disease) put his foot down, refusing to do anything further, because he was asymptomatic.
2. If you are between 55 and 69 years of age, it’s tough.
If the serum PSA is found high, and a prostate cancer that would have killed you if undetected is found early enough, it would have saved your life. But if your serum PSA is mildly high, you will land up going through multiple tests, whose results may create even more confusion, with perhaps an unnecessary biopsy, and if you are found to have prostate cancer, like my doctor friend, leading to a bouquet of choices that are confusing even to doctors, forget about non-doctors.
Unless you have the physical, monetary and mental resources to navigate the healthcare system if your screening serum PSA level is found high, when you are asymptomatic, including access to trusted high-quality physicians and surgeons, and the mental make-up to make rational decisions without freaking out and stressing daily, don’t do a serum PSA level.
This also means that if and when you go for those often unnecessary, whole body executive health check-ups (you do need annual check-ups, but not an entire array of tests of no proven use), do not allow a serum PSA test to be done, unless you are sure you want to know the result and can handle the consequences of an abnormal result.
Footnotes
1. Jahn JL. Int J Cancer 2015;137:2795.
2. https://www.cancer.gov/publications/patient-education/prostate-cancer-treatment-choices.pdf
3. US Preventive Services Task Force JAMA. 2018 May 8;319(18):1901-1913.
4. https://gco.iarc.fr/today/data/factsheets/populations/356-india-fact-sheets.pdf
5. Ghose A et al. Korean J Urol Oncol 2020;18:170
Last Week

Other Cancer Screening Topics
Atmasvasth Newsletter
Join the newsletter to receive the latest updates in your inbox.